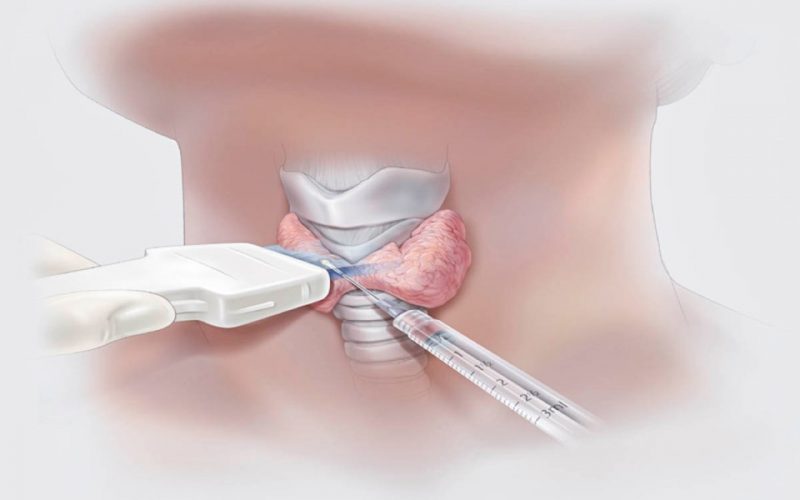
The main purpose of a biopsy is to establish which process we are dealing with: a benign or malignant tumor. After taking a tissue sample, carry out microscopic and histochemical examination.
“Your biopsy has been sent for histological analysis,” is a phrase that is familiar to many of us. What’s behind it?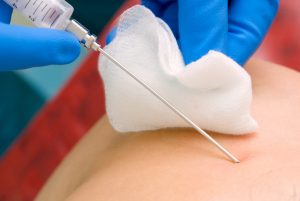
A biopsy is a diagnostic procedure in which tiny tissue particles (biopsy) are taken from a “suspicious” place, for example, a tumor, a polyp, or a sore that does not heal for a long time. Different instruments are used depending on where the biopsy comes from. This can be a thick needle, an endoscope (when examining the esophagus or stomach), a light guide (during bronchoscopy), a regular scalpel (during a surgical operation).
The main purpose of a biopsy is to determine whether a benign or malignant process is to be fought. This procedure is also used when monitoring the treatment of cancerous tumors. Taking a biopsy correctly is a special art that requires experience and skill from the doctor. The result of the analysis and, accordingly, the choice of treatment tactics depend on the accuracy of his choice (at the beginning of its existence, a malignant focus is quite tiny).
Pieces of tissue obtained with the help of biopsy are sent to a special laboratory, where their histological analysis is carried out. It is based on the fact that all cells of the body have a characteristic structure, depending on which tissue they belong to. With malignant degeneration, the picture changes dramatically: the internal structure of the cell is disrupted, it ceases to be similar to its neighbors. These disturbances are usually so significant that they can be seen with an ordinary microscope.
But before considering the material taken during the biopsy, it must be processed in a special way: cut into very thin transparent slices (they are called slices) and stained. To prepare sections, a piece of tissue is first made hard (for example, impregnated with paraffin), and then, fixed in a special holder, cut with a special super-sharp knife – a microtome.
The resulting thin films are placed on small oblong glasses and dyed directly on them. There are quite a few dyeing methods, but they have one thing in common – they are all carried out in several stages. Previously, preparations were transferred from bath to bath by hand, now all stages of staining can be carried out by special devices. But this is perhaps the only stage where automation is possible. All the rest entirely depend on the skill and attention of specialists.
When the stained specimen is under the eyepiece of the microscope, a pathologist, a doctor of extremely important specialization in medicine, steps in. After assessing the features of the cells under study, he makes his own verdict: benign or malignant tissue was taken for biopsy. Moreover, depending on the type of cancerous “breakdowns” of cells, it is often possible to determine the type, features and even the prognosis of the disease.
When research under a light microscope is not enough, they resort to immunohistochemical research. In this case, the sections are treated with several (in each specific case, different) antitumor sera. If the “direction” of any of them coincides with the nature of the tumor, yellowish granules appear in the cells of the preparation, clearly visible under a microscope. So, this method has proven itself well in the diagnosis of melanomas https://en.wikipedia.org/wiki/Melanoma – malignant skin tumors that easily metastasize.
In some cases, when it is necessary to understand what changes have occurred in the “internal organs” (organelles) of cells, electron microscopy comes to the rescue. The huge magnification (up to 100 thousand times), which gives an electron microscope, has its advantages and disadvantages: allowing you to see even large molecules, at the same time it is able to keep only a few cells in the field of view. This increases the importance of how accurately the material was taken for research (both during the biopsy and during the preparation and selection of sections).